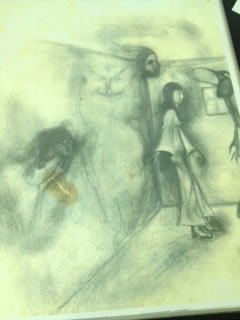In his quiet, modest way, Glenn was proud of his robot. It was 1974, at a local high school science fair in Boca Raton, Florida, and Glenn, a 15-year-old sophomore, had spent months painstakingly constructing a jumble of wires and circuits on wheels with three arms, each containing a photosensitive panel. He called it a “light-searching, maze-overcoming robot.” The contraption would circle around inside a box until one of the arms detected light, in the form of a bulb Glenn placed at different locations. Then it would move towards the light, circumventing the obstacles that Glenn put in its way.
Someday, Glenn explained to the judges, this kind of technology could be used to mow lawns, even to transport equipment on a lunar terrain in a future space mission. The robot won several prizes, and the next year, Glenn updated the project and won yet more awards in Colorado, where his family had moved. Impressed, one of the judges wrote a letter to Glenn urging him to pursue electronics as a career. In a photo that appeared in the local paper, he is wearing a neatly pressed, button-down shirt and is resting one hand on the robot he created, a hint of smile in the corner of his mouth.
Glenn’s younger sister, Tamara, wasn’t surprised at his success. Her brother’s gifts extended far beyond math and science. He learned Russian in high school because he was curious about the language, and he had a flair for art, drawing cartoons and painting portraits and landscapes, a few of which he managed to sell. “Glenn is without a doubt a fine talent,” one teacher wrote on an evaluation. “It’s quite nice to see someone this young developing a personal style.” He wasn’t always at ease with other kids, which made the family’s moves—from Colorado to Florida and then back again—difficult for him. But with Tamara and his parents, Earl and Barbara, he was gentle and had an impish sense of humor, playing pranks on his sister and sharing quips from Mad magazine, which he devoured as soon as it arrived in the mail.

Then, when he was around 17, Glenn abruptly started spending long hours in his room. He stopped talking much, even around his family. One day, Tamara remembers, Glenn went into his room and spent hours destroying his belongings, including his treasured collection of every single Beatles album. On another night, Barbara came home to find Glenn sitting on the floor of the dining room. He’d carved a cross into the wall with a knife, and wouldn’t respond when she spoke to him. Glenn’s parents sought help from their family physician and a series of psychiatrists and social workers. At first, doctors thought he had bipolar disorder and depression, but after a few months, a psychiatrist hit on the correct diagnosis: Glenn had schizophrenia.
For the next few years, Glenn shuttled in and out of hospitals while his parents searched desperately for doctors and treatments that might help him. Sometimes, in the middle of the night, he would start shouting for no apparent reason, or begin talking feverishly about angels and demons he believed were communicating with him, possibly through electronic devices. His doctors prescribed medications that sometimes helped suppress the delusions but had severe side effects; therapists and counselors, with varying degrees of enthusiasm, tried to teach him to distinguish between fiction and reality. But the common message from virtually everybody who worked with Glenn was that his life was basically over. He wasn’t going to become a world-famous engineer or travel to the moon. He wasn’t even going to finish high school.
And that’s pretty much how things worked out. During one lucid period, while medications were suppressing some of his psychosis, Glenn managed to obtain a G.E.D. But he never went to college and never held down a job. Instead, he lived on disability checks while shuttling between subsidized housing and group homes for the mentally ill. Depending on whether he was taking his meds, his delusions came and went. He smoked compulsively. He would become so obsessed with some all-consuming idea, frequently related to the Bible, that he wouldn’t wash, he would let his living environment become filthy, he wouldn’t eat. If it hadn’t been for his mother, who kept a close watch on him, he might have ended up on the streets.
Throughout all this, Tamara Sale, who is three years younger than Glenn, took on the role of the unfailingly levelheaded sister. (Tamara asked us not to use Glenn’s last name in this story.) When her kind, funny, creative brother was overtaken by paranoid outbursts, she tried to calm him without betraying her fear. She became deeply distrustful of mental health professionals, who, at various points, told Glenn he shouldn’t try to get a job and urged the family to stop supporting him financially (advice his parents ignored.) Tamara felt a kind of survivor’s guilt as she achieved milestones that her brother would never experience: finishing school, getting married, starting a career. “Psychosis was a sort of earthquake in our reality,” she explained. “Just like with a major earthquake you find yourself not trusting the earth you’re walking on, the same is true for psychosis, both for the person who experiences it and for the people close to them.”
Tamara eventually settled in the suburbs of Portland, Oregon, where she worked for a local mental health agency. It was through her work that, in the early 2000s, she heard about a radical new approach to schizophrenia that had been developed by researchers in Australia. Tamara was shocked to discover that this program took a very different attitude toward schizophrenia than nearly everyone who had treated her brother. Over and over again, Tamara and her family had been told that schizophrenia was a hopeless condition. By contrast, these Australian researchers were convinced that with the right kind of treatment, delivered at the right time, many sufferers could lead pretty normal lives.
This treatment method was based on a simple question that has upended everything that scientists once thought they knew about schizophrenia: What if its most destructive symptoms, the ones that had swallowed Glenn’s personality and ravaged his life, could actually be prevented? In other countries, this method is changing people’s lives in ways that psychiatrists had never imagined possible. But in the U.S., it has barely expanded beyond a handful of academic and specialty centers. Even among doctors and mental health professionals, surprisingly few people seem to realize that such a potentially transformative approach to this terrible disease even exists.
Not many people would include schizophrenia on a list of major diseases that burden American society, but that is what it is. Schizophrenia affects about 1 percent of the population, roughly three times the number of Americans who suffer from Parkinson’s. Because the disease typically appears in adolescence or early adulthood, it claims many more years of healthy life than conditions like leukemia and HIV. Its sufferers also die earlier, about 12 years before the typical American. Economists say that schizophrenia costs the U.S. at least $60 billion a year, and probably a good deal more. We pay for the many forms of assistance that people with the condition require, and we pay for what happens when they don’t get the help they need. More than 40 percent of all people with schizophrenia end up in supervised group housing, nursing homes or hospitals. Another 6 percent end up in jail, usually for misdemeanors or petty crimes, while an equal proportion end up on the streets.
Among researchers, schizophrenia has long been known as the “graveyard of psychiatric research.” In the 1890s, when the German psychiatrist Emil Kraepelin began coming up with categories of mental illness, he devoted one diagnosis to a peculiar madness that seemed to appear in the late teens and early twenties, a combination of delusions, hallucinations and major cognitive impairment. It was then known as “dementia praecox”—literally “premature dementia,” which was consistent with Kraepelin’s understanding of an irreversible unraveling of the mind. About ten years later, the Swiss psychiatrist Eugen Bleuler gave the disease its name, forming the word from the Greek roots schizein, which means “splitting,” and phren, which means “mind.” Bleuler identified four categories of symptoms that psychiatrists still use today—abnormal associations, autistic behavior and thinking, abnormal affect, and ambivalence. These insights, however, did not lead to any great advances in treatment. Bleuler and many of his contemporaries, all disciples of Freud, tried psychotherapy, while others experimented with lobotomies and inducing seizures in an attempt to “shock” schizophrenia out of the body. Regardless of the method, the end result was usually lifelong confinement in an institution.
It wasn’t until after World War II that scientists started to understand the biological basis of schizophrenia. They zeroed in on dopamine, the chemical that carries signals in the brain that affect both movement and emotions. Drugs that blocked some of the brain’s dopamine receptors stopped the delusions and hallucinations, reducing and sometimes even eliminating the outward signs of madness. The introduction of chlorpromazine, marketed as “thorazine,” eventually fueled calls for de-institutionalization, since the drug made it possible for people with schizophrenia to rejoin their communities without engaging in visibly psychotic behavior.
But this revolution went only so far. Antipsychotics (including newer, second-generation versions) cause severe side effects, from muscular and movement disorders to weight gain. This is one of the main reasons that 40 percent of people with schizophrenia stop taking their medications within 18 months. And while antipsychotics can help schizophrenia’s “positive” symptoms, such as hallucinations, they have a minimal impact on the “negative” symptoms, which are arguably more devastating. People who have schizophrenia can lose the ability to focus, to sustain effort, to carry on a conversation or to maintain eye contact. They become progressively untethered from normality. And as they lose the very essence of their personality, they often alienate the people who care for them. It doesn’t happen that way for everybody; for reasons researchers don’t yet understand, some people actually recover fully on their own. But through the 1980s, the prevailing assumption among mental health professionals was that the vast majority of people with schizophrenia would never lead anything resembling an independent life.
The discoveries that would challenge this conception came, as they often do in medicine, somewhat by accident. Over the years, researchers had found that in people with schizophrenia, important parts of the brain are larger than usual, including the prefrontal cortex, which controls decision-making. Gray matter—the neural connections on which electrical signals travel, forming thoughts and emotions—is thinner. But the researchers who discovered this were mostly looking at people who had been struggling with the disease for a while. As a result, they didn’t know whether these differences in the brain were caused by the disease, the medications or both.
When they began studying people who had developed symptoms only recently, they found that the changes to the prefrontal cortex and gray matter were far less pronounced. Patients were more sensitive to medication, which meant that the standard high doses created more debilitating side effects—and that low doses would be more than adequate to control hallucinations and delusions. Newly diagnosed patients also responded better to cognitive therapy to help them deal with irregular thoughts. Eventually, researchers homed in on a key variable: the duration of untreated psychosis, or D.U.P. They theorized that the shorter the interval between the first appearance of symptoms and when a person gets treatment, the greater the chance of some form of meaningful recovery.
One of the first psychiatrists to put these insights into practice was an affable Australian named Patrick McGorry, who was working at a research hospital in Melbourne and was horrified at what happened to schizophrenia patients there. “It was terrible,” McGorry told me. “They were getting 10 times the medication they needed, and given nothing else, and just being chucked back into the community. Maybe the antipsychotic drugs controlled some of the irregular thoughts, but their lives were in ruins.” In the late 1980s, McGorry decided to try and minimize the gap between the appearance of symptoms and treatment. First, that meant identifying the disease as early as possible. The most conspicuous initial signs are delusions or hallucinations. After some time—weeks, months or a few years—people with schizophrenia lose “insight.” That is, they can no longer recognize that the strange voices and visions they are encountering are not real. Eventually, they start to have psychotic breaks—extended periods of time when they lose insight in ways that make normal functioning impossible. At the time, the vast majority of people didn’t receive any treatment until at least after the first break.
McGorry and his colleagues eventually developed a lengthy questionnaire that clinicians could use to screen for the warning signs of psychosis. Once potential sufferers had been identified, the treatment offered by his clinic “wasn’t really rocket science,” as McGorry likes to say. It combined low doses of medication for those who required it with a more comprehensive and diverse set of services than psychiatry has traditionally offered. These included therapy and coping techniques to help schizophrenia patients finish school or keep their jobs—interventions intended to stop the downward spiral from which so many people never recover.
This strategy, which McGorry and others dubbed “early intervention,” was cutting-edge in the world of mental health. And yet it actually operates on the same logic that doctors have used for decades to reduce the incidence of serious physical illnesses. To fight heart disease, for instance, doctors screen for high blood pressure and prescribe medication to control it. But they also counsel people on how to avoid weight gain through diet and exercise. Since 1972, the death rate from coronary heart disease has fallen by roughly half—and researchers think basic preventive care has done as much to achieve that reduction as advances in surgery have.
The concept, however, has only recently been applied in psychiatry. Historically, severe mental illness was typically treated only in its advanced stages by hitting it with massive doses of drugs, combined with therapy, and assuming there was not much else to be done.
McGorry eventually developed a specific analogy between schizophrenia and cancer. Physicians think of cancer as having distinct stages—from stage 1, when early detection can make a huge difference in survival rates, to stage 4, by which point the cancer has spread and the focus usually shifts to managing the patient’s inevitable decline. In McGorry’s conception, schizophrenia goes through a “prodrome” stage when symptoms gradually emerge, a “first episode” phase that covers, on average, the two years before the first break and finally a “chronic” phase when the disease causes a steady deterioration in many patients that can be difficult if not impossible to reverse. By reaching people in the first or second stages, McGorry argued, psychiatrists could prevent the disease from reaching its most destructive form. “All we ever saw in the ‘80s was the equivalent of stage 4 schizophrenia,” says Ken Duckworth, a psychiatrist and medical director of the National Alliance on Mental Illness. “It would be as if you were an oncologist, and all you saw were people with metastatic breast cancer.”
In 1996, McGorry and his colleagues published some early findings in a 1996 paper for Schizophrenia Bulletin. Compared to schizophrenia patients on the whole, Australian researchers said, those who went through the Melbourne clinic spent about half as many days in the hospital. They also scored better on some (although not all) standard psychiatric evaluation tests, displaying better relationships with family and friends and retaining traits like motivation and empathy. Around the same time, researchers across the world, in Denmark, the United Kingdom and the U.S., were coming up with similarly encouraging findings. 1 Diana Perkins, a psychiatrist who has been running an early intervention program at the University of North Carolina for about 10 years, told me, “I used to treat clinical schizophrenia and I wasn’t expecting people to get better like this. With this kind of psychosis, it just didn’t happen.”
The voices were faint at first. Psssst. Psssst. But soon they grew louder, more insistent, and more ominous. You’re ugly. You’re so hideous. You’re a pervert. You’re horrible.
In 2012, Mar J (who asked me not to use her real name in this story) was 21 and living with in New York her mother. She hadn’t had an easy life. She grew up in a housing project in a large family, and was abused by a relative. But she’d made it through high school and was in her second year of college, studying criminal justice. She still remembers the day she started hearing the voices. “It fell on me,” she says simply. “That’s how it felt.” Sometimes the voices made kissing sounds, or moaned like they were having sex. Sometimes they argued with each other about whether the dress she was wearing was pretty. Eventually they became a nonstop dialogue inside her head, making it impossible to even complete a thought.
A psychiatrist determined that Mar J had schizophrenia and gave her an article about the disease, along with a prescription for antipsychotics. The pills, she said, made her feel “zombified”—she’d sleep for two days straight and drool uncontrollably, and her leg became so numb she started walking with a pronounced limp. After her insurance stopped paying for her therapy, Mar J stopped taking her meds. That's when she had her first psychotic break.
One evening in 2013, she became convinced that her friends and classmates were plotting to ruin her in school. She drove her car to several of their houses, got out and started screaming: “You’re wicked witches! I know what you are up to!” At one house, a man came outside, told her to shut up and eventually punched her in the face. She tried to run him over, swiping two parked cars and severely damaging her own in the process. When she got home still very much in the throes of psychosis, her mother called the police, who took her to a mental hospital.
There, Mar J got high dosages of medication and a referral to an outpatient clinic, where she says the staff did little except offer her more meds. Nobody mentioned the possibility of her returning to her studies. Within a few weeks she was hearing the voices again and writing Bible verses on the walls of her mother’s home to “keep the demons out.” She landed back at the hospital, but this time, she didn’t bother going to the outpatient clinic.
It was the third psychotic break that changed her life. After getting in a fight with her mother, Mar J took her car and drove from the Bronx to Queens, sleeping for several nights in shopping mall parking lots. She asked for jobs in fast-food restaurants and used their bathrooms to wash up. When the voices got too loud, she’d start driving again. On about the fifth night (Mar J doesn’t remember all the details) she drove into Manhattan and up to 168th Street on the West Side. When she peered into other cars, the drivers were people she knew. She was sure that some of them were following her.
Eventually, Mar J made an illegal turn right in front of a police officer, who pulled her over and discovered that her mother had reported the car as stolen. But instead of arresting her, the officer called her parents, who admitted her to the New York Psychiatric Institute. This time, she got a referral to an early intervention program called OnTrackNY.
First, a staffer established that Mar J was under 30 and that her first psychotic break had happened within the last two years. She then started attending sessions twice a week, with staffers working closely with her to devise a treatment plan. This is a core principle of early intervention known as “shared decision-making,” and is intended to help patients feel more invested in their care. A dedicated psychiatrist switched her to a lower-dose medication with fewer side effects. A therapist helped her develop strategies for coping with her delusions. Staffers have also accompanied her to court to settle the traffic violations from that night of driving around Manhattan, and have contacted her school to make special arrangements for her disability. In addition, Mar J works with an employment counselor who has set up job interviews and helped her prepare for them. Sometimes they go for coffee at Panera Bread and talk about what she wants to do after she graduates from college.
Mar J will complete the two-year program soon, although staff members remain available after that for phone calls and consultations. In the future, her well-being will depend in no small part on her determination to maintain her treatment regimen and to seek help when she needs it. The people working with Mar J told me that she has missed almost no appointments, even though her commute entails more than two hours of bus and train rides each way. “We see patients getting better and better,” says Nannan Liu, Mar J’s therapist. “I wasn’t taught that way, like this was something we could do on regular basis.”
When I first met Mar J in June at the OnTrackNY offices on the Upper West Side, she was dressed neatly in shorts and a button-down top, with black curly hair that fell lightly over her ears. She looked me in the eyes as we spoke, smiling frequently and sitting up almost absurdly straight. Last year, she got nearly all A’s, and this semester she is taking five classes instead of the usual three, to make up for the time she lost to the disease. A few months before we met, she’d won a major speaking part in a play for a small theater company (her therapist came to the opening night). Mar J says she might like to work in law and is also building her own website to help people who have schizophrenia. She still hears the voices, she told me, but with her therapist’s help, she is learning to ignore them. “The thoughts come in a wave. You can’t stop them. You just have to let the wave flow,” she explained. “You just have to let them go. ‘Oh, there goes a thought, just keep it going.’ Kind of like a hiccup or a burp.”
Listening to Mar J, I was struck by how much she had in common with Glenn. They were both bright young people overtaken by a terrifying illness. But while Glenn had never recovered, it seemed very possible that Mar J could live with the disease while still remaining herself.
In July, I traveled to Oregon to meet Glenn’s sister Tamara, who is now a director of the state’s early intervention initiative—the Early Assessment and Support Alliance. We sat in her Portland office, with views of the downtown skyline and the Cascade Mountains filling the large windows. Tamara has round facial features; she nods a lot while listening and speaks in soothing tones. “I had been actively trying to understand what would have helped Glenn, for many, many years—really my whole adult life,” she explained. As she learned more about early intervention, she said, “I realized that it was making real the alternative story that I had written in my own head—what could have happened in our own lives.”

EASA is one of the oldest early intervention initiatives in the country. Its treatment regimen is very similar to that of OnTrackNY, but it makes a particular effort to reach people well before they’ve had a psychotic break. Staffers educate schoolteachers, community college instructors, health care providers and law enforcement officials about the warning signs of psychosis, like abrupt withdrawal, loss of interest in work or school or irrational-sounding public outbursts. (The current holy grail in psychiatric research is to develop a blood test or some other method of identifying people likely to get schizophrenia. But some experts and advocates worry about over-diagnosis, over-medication, and other negative consequences of finding and possibly treating the disease before symptoms even appear.)
At EASA’s Eugene office, which operates through the PeaceHealth Medical Group, I met a charismatic 25-year-old peer support specialist who asked to be referred to as Archer. He went through the program himself after developing schizophrenia six years ago. The program, he says, “completely turned my life around from somebody who couldn’t leave my mother’s basement. I thought I was going to be there forever.” Archer’s experience gives him an unusual insight into how to reach patients who have trouble communicating in formal settings. He likes to play the guitar with those who have an interest in music, and he’s noticed that people struggling with psychosis find it easier to talk on long car rides. “There’s something about looking through a car windshield, and having that side-to-side conversation rather than face-to-face,” he explained.
Nearly a decade after McGorry and his team published their preliminary findings, there is now a solid body of scientific research supporting the value of early intervention. Just this summer, a breakthrough study from researchers at Yale showed that early intervention actually saves money, in part because people who get the services are far less likely to need expensive hospitalizations. Within the EASA program, the rate of hospitalization among patients has dropped from nearly half of participants in the first three months to about 5 percent after 18 months. Lisa Dixon, the Columbia University psychiatrist who designed and oversees OnTrackNY, cautions that because early intervention is still comparatively new, there’s less data available on how patients fare later in life and how best to support them over the long term. But the results are sufficiently promising that national health care systems of the U.K. and Australia provide extensive early intervention services. They’re also widely available across Europe and in Canada.
Here in the U.S., it’s a different story. Robert Heinssen, a top official at the National Institutes of Mental Health, points out that even though American researchers played pivotal roles in the research and development of early intervention, only a relative handful of programs have actually provided treatment services. In January 2014, after the Sandy Hook Elementary School massacre in Newtown, Connecticut, several lawmakers approached NIMH and the National Alliance on Mental Illness for advice on how to improve treatment of people with mental disorders. 2 The experts recommended putting more money into early intervention. Congress earmarked $25 million in matching funds for states that started their own programs. But even if every state takes its share of the money, this will only be enough to create about 100 early intervention programs throughout the entire country.
It will come as no surprise that one reason the United States lags so far behind the rest of the world is its deeply dysfunctional system for financing medical care in general, and mental health care in particular. In other countries, national health care systems have broad authority to set priorities and budgets. Officials can respond more quickly to emerging research and take a longer-term view of social investments because, unlike insurance companies, they don’t have shareholders to please.
The Affordable Care Act provides more Americans with access to insurance. 3 But private insurers in the U.S. aren’t equipped to handle serious psychiatric illness and would just as soon avoid having to do so. They hand mental health care off to “carve-out” firms that tend to push cheap, simple treatments like medications while skimping on labor-intensive but more effective treatments like therapy and support, even when those methods can save more money over time. And even though insurers are supposed to cover all mental health services that are “medically necessary,” the companies have a great deal of leeway over what qualifies. Services that many researchers now believe are crucial, like assistance with staying in school or holding down a job, may not be eligible for reimbursement. “When you bill for things, you have to have a code for everything,” says Perkins, the UNC psychiatrist. “You can’t really do that for something like vocational services.”
There’s also a deeper problem at work. Too many people, including some mental health professionals, think of psychiatric disease as something fundamentally different from physical disease. And yet the more we learn about mental illness, the less meaningful that distinction appears. McGorry now believes that the model of screening, preventative care and aggressive early treatment could be used to reduce the incidence not only of schizophrenia, but of other mental illnesses like depression and bipolar disease. He has spearheaded a government-funded initiative to create “Headspace” centers all over Australia—drop-in clinics where teens and young adults can go without a referral from a doctor and get free counseling or treatment for all kinds of mental issues. “Seventy-five percent of mental disorders appear by age 25,” he says. “An awful lot of that is in teenagers or young adults.”
The U.S. may be far from introducing anything so forward-thinking, but there are modest steps that policymakers could take right now that would make a significant difference. Under the Affordable Care Act, state and federal regulators could mandate that insurance companies cover all aspects of early intervention services. If Congress doubled or even tripled the money it set aside for early intervention in 2014, that would still cost less than $100 million a year—barely a dent in the federal budget. Policymakers could also recognize, in the form of research funding, that the toll of mental illness rivals that of many other diseases. Right now, for every dollar that the federal government spends on medical research through the National Institutes of Health, 16 cents goes to HIV/AIDS, 11 cents goes to cancer, and less than four cents go to all mental illnesses combined.
In my conversations with Tamara, I was often reminded of how directly these policy choices shape people’s lives. One afternoon in July, Tamara and I went to meet Glenn, who is now 57 years old, at a park he likes to sit in. It has a swingset and a picnic area and tall, leafy trees that cover most of the grounds with shade. Glenn wore an old navy blue racing jacket, with torn elastic cuffs and racing stripes down the arms that were peeling off, and black sweatpants with holes in them that looked about a size too big. Clumps of wispy hair matted down to a few spots on his balding head. His thick beard was white, except for the burnt orange tint of tobacco around his lips. While we spoke, he swigged frequently from a plastic bottle filled with a yellowish liquid and some grains at the bottom—tea leaves and coffee grains that help ward off the evil spirits, he explained.
Psychosis comes and goes. A few years ago, Glenn was in a ham radio club and talking seriously about working on some of his inventions; in family photos from that time, his appearance isn’t so unkempt. When his father died in 2013, Glenn was too sick to travel. Tamara thinks his sense of loss may have triggered his latest lapse. He now lives in a group home where he gets attentive, loving care, and where they honor his long-standing wish to stay off medication. On most days, he spends his waking hours feeding birds, listening to Bible verses on a tape recorder, and researching his current interests, which include the possibility of people coming back from the dead and a technology called “Voice to Skull” that, according to Glenn, angels and evil spirits use to send messages into people’s brains. “It could be a way for fallen angels to talk to people, and holy angels too,” Glenn told me. “The Apostle Paul saw a light called Jesus talking to him. And the Bible says God is light. And radio is part of the light spectrum. So Voice to Skull may be a way for Jesus to talk to people.” (Although, he confided, he couldn’t be sure college students weren’t using the technology to impersonate angels, as a prank.) Glenn was kind and courteous, and although he mostly looked down or off into the distance as he talked, every so often he’d give me a gentle glance through his bright green eyes. He showed little emotion, even when he appeared frustrated with Tamara because she hadn’t, as he’d requested, notified the Federal Communications Commission about Voice to Skull.
Later, Tamara told me that, for all her brother’s struggles, she sees him as an inspiration, and always believes that he could one day get better. “Every bit of happiness and friendship that he experiences, every conversation we have, I value deeply,” she said. Sometimes, though, she finds herself thinking about what might have happened if Glenn had gotten the same kind of care that the young patients in her program do today. “He was very smart, very intelligent. He’s interested in learning. He wanted to finish school, he wanted all the things that other people want. He wanted to work, he wanted a girlfriend, you know?” More than anything, her work has taught her what becomes possible when doctors treat a person with mental illness as a person with a future.
Artist's Statement
I was diagnosed with schizophrenia when I was 19. I've been living with the mental disease for about 15 years now. Since then, I've been on two different medications and had quite a few relapses from the wrong medication. I'm heavily medicated and go to my psychiatrist once a month. Making art helps my symptoms when I'm not feeling well. It's a form of catharsis and release from all the confusing emotions and thoughts that I go through on a daily basis.
About the Art: The circle in the center represents "self." The lines represent the voices and the ghostly faces are the hallucinations. The different colors are the different stages, from alert to paranoid state. The chaotic background, along with the lines, represents the confusion from rational and irrational thought, level of stress and anxiety.
—Glen Brown.