All the lights were off in the used RV that night, and the blinds were closed to prevent anyone from seeing inside. Five people huddled in the small main room. Kate Petty, 34, lay on a bed that had been converted from a fold-down dinette table, underneath a large painting of a leopard. Her husband, Caleb, whose beard and long hair is the same auburn color as Kate’s, sat by her head and clutched her sweaty hand. She had been in labor for more than 24 hours and she was breathless, exhausted. The only light in the RV came from a flashlight held by a woman standing on Kate’s left. Another woman crouched between her splayed legs, hands outstretched.
“Keep going, honey. You got it,” said the woman with the flashlight.
Kate groaned. Her baby’s head emerged into the quivering circle of light.
“Is he stuck?” she asked in fear.
Kate’s contractions had started on the morning of May 8, 2017, in the Pettys’ brick one-story home in Opelika, Alabama. After two pregnancies, Kate knew she had some time to kill, so she made a last-minute grocery run. When the contractions picked up that evening, she and Caleb hopped in their car and headed for the Georgia state line, a half-hour drive away.
The roads wound through soft, wooded hills until finally the couple saw the large wooden cross marking the entrance of 3 Creeks Campground. They’d picked 3 Creeks for two reasons: It was close to Alabama, and it had working sewage. “A really podunk hole in the wall,” was how Kate described the place. The RV was waiting for them in slot K-9, already stocked with the supplies they’d need: old blankets, towels, Chux pads, buckets, candles, raw honey for energy. That night, the contractions were coming about every five minutes but Caleb and Kate curled up together on the bed and managed to get some sleep.
By morning, Kate couldn’t talk through her contractions anymore. She got into the rose-patterned birthing tub that her doula, Ashley Lovell, had filled with water from a plastic hose. Kate’s midwives, Rachel Hart and Paige White, arrived around 9 a.m. During a check, they realized the baby was asynclitic, or entering the birth canal at an angle. They had Kate get out of the tub and move into different positions to align the baby’s head. Everyone took turns rubbing Kate’s back and fanning her face. Meanwhile, Kate’s mother, Elizabeth Landreth, and other relatives sat on John Deere chairs outside, waiting. The campsites at 3 Creeks were close together, so it wasn’t long before some of their fellow campers became aware of what was going on.
It was hot in Georgia in May and the midwives were cranking the air conditioning, but the breaker kept tripping and Caleb had to hop in and out of the camper to get the power back up. It got so hot in the RV, Kate wasn’t sure she could stand it. She could hear a group of guys who worked for the Georgia Power utility company grilling and drinking beer and cutting up outside. The campground’s owner came by to lend Caleb a hand with the breaker. At one point he was standing right by the window, about 5 feet away from Kate. The couple hadn’t told him they planned to give birth at his campground and weren’t sure how he would react. So every time Kate had a contraction, the midwives closed the windows to muffle her cries. “I was pretty loud, I feel like, but he had no idea,” Kate said.

Every so often throughout the day, the midwives used a Doppler fetal monitor to detect the heartbeat. To help the labor progress, they had Kate squat, sit on a birthing stool and try the McRoberts maneuver, in which she lay on her back and pressed her legs to her belly. As the light faded and Kate neared the 30-hour mark, she started to panic. She had been in labor for so long. She worried she didn’t have the energy to keep going. She asked if she should go to the hospital for a cesarean section.
But Hart knew the baby was close. She told Kate that she wouldn’t stop her from having a C-section if that’s what she wanted, but she wasn’t going to tell her to have one, either. Instead, she asked Kate to get on her back. She felt like a turtle stuck the wrong side up. At Hart’s direction, Caleb held one of her legs in the air. A painful contraction came, and then another, and then the baby was coming so fast that White didn’t even have time to get her gloves all the way on.
“Here he is! Here he is!” she cried. At 8:03 p.m., a full day after Kate and Caleb had arrived at the campground, their son Jett was born and soon announced his arrival with a wail. To Elizabeth, standing anxiously right outside the window, it was the most beautiful sound she’d ever heard. “Oh, my baby,” she heard her daughter say. Elizabeth started jumping up and down with joy and relief; around her, the campers who knew what was going on inside the RV clapped and cheered in the humid night.
There are women who prefer to use a midwife because of deeply held beliefs about religion or wellness. And then there are those like Kate, who are simply desperate to avoid having a baby in a hospital. Mothers in this latter category have often endured a traumatic hospital experience and fear being pushed into risky procedures or surgery if they deliver there again. These fears are hardly unfounded in Alabama, which has one of the country’s worst rates of infant mortality, with maternal mortality also on the rise.
When it comes to women’s reproductive choices, we think of the primary battlegrounds as contraception, sex education and abortion. We hear far less about the significant restrictions on childbirth. While midwifery care is mainstream in other Western countries, it’s relatively rare in the United States. The closest option is a nurse-midwife—a registered nurse with a midwife credential who mostly operates in hospitals under the authority of doctors. This is a very different experience from having a trained midwife supervise a delivery in the home or in a birthing center. In some places, it’s impossible to access such services without skirting the law. Seventeen states, including North Carolina and Illinois, have laws that put midwives at risk of criminal prosecution for assisting birth outside a hospital. In Alabama, midwives were not permitted to practice in the state during Kate’s pregnancy.
And so, each year expecting mothers jump the border into Tennessee, Mississippi or Georgia, where midwifery is either legal or at least exists in some kind of gray area. Whether the journey is 10 minutes or two and a half hours, these women often make the drive while already in labor and pray they aren’t forced to have the baby in a parking lot or by the side of the road. They give birth in makeshift spaces, often in secret—Airbnbs, cheap hotel rooms, campers, a network of birthing cottages nestled anonymously throughout the hills of small, southern Tennessee towns, the western part of Georgia or along the Mississippi line. These might not be places where most mothers would want to give birth, but they give women like Kate something far more precious: a greater measure of control over how they bring a child into the world.
Alabama has a rich tradition of midwifery, but it is one that has virtually been erased from living memory. As in most places in the United States, until the mid-1800s it was midwives who were responsible for delivering children. Birth was something that happened in the home, among women. To this day, midwives still refer to their work as “catching babies”—reflecting a belief that birth doesn’t require medical intervention under normal circumstances, just a pair of hands to safely collect the child.
But as medicine became professionalized, its leading practitioners took a very different view. In 1915, the influential obstetrician Joseph DeLee declared that midwifery was a “relic of barbarism.” He also called on physicians to save women from the “pathologic” process of labor using sedatives, forceps and episiotomies—the surgical cutting of the perineum. By the early 1930s, nearly two-thirds of births in the U.S. happened in a hospital.
There was one place where midwives remained crucial: the South. During Jim Crow, black families could not access white hospitals and white doctors often refused to treat them, so it fell to black “granny midwives” to deliver children. In Alabama, Margaret Charles Smith caught her first baby at the age of 5 and, in her own telling, went on to deliver 3,500 children without losing a single mother. She once described saving an extremely premature baby by making an incubator out of a cardboard box and hot water bottles. Onnie Lee Logan started practicing in 1931, delivering nearly every child born in one black Mobile suburb. “I do all my work keepin em from having lacerations and havin to have stitches,” she recounted in her book, explaining how she used hot towels to stretch the skin and how she knew exactly when the mother should start pushing so the baby was positioned correctly.
The 1964 Civil Rights Act, as well as the introduction of Medicare and Medicaid, eventually led to the integration of medical services. By the 1970s, 99 percent of American births took place in hospitals and states were passing laws preventing midwives from practicing, ostensibly for health and safety reasons. Alabama ended the legal practice of lay midwifery in 1976. A tiny number of home birthers persisted, mostly white, middle-class women seeking an alternative to the hospital. It was technically a misdemeanor for midwives to assist them, but the likelihood of being prosecuted seemed slim.
One woman who defied the ban was Karen Brock. She’d delivered hundreds of babies since the 1980s, following the example of her midwife grandmother. In 2002, Brock was attending a birth that was complicated by a ruptured uterus and cord prolapse, which occurs when the umbilical cord drops through the open cervix into the vagina. She rushed the mother to the hospital, where the baby died. According to Brock, the doctor said her actions saved the mother’s life, but she was charged with the misdemeanor of practicing nurse midwifery without a license and pleaded guilty.
Brock, 61, is petite with straight silver hair and an abiding affection for Chaco sandals. She told me that at the time of her arrest, she didn’t want to abandon the 27 Alabama families still in her care. So she decided to move her practice to Tennessee, where she could operate as a certified professional midwife. (Certified midwives do not have to be nurses, but undergo training and apprenticeship programs.) For a couple of months, she delivered babies in a trailer in a midwife’s backyard. Then she rented a house in a small town right on the Alabama border. After about five years, she received a cease-and-desist order from the state of Tennessee for running an unauthorized birth center. (The state defines a birth center as any building “exclusively or primarily” dedicated to birth.)
The day she received the order, Brock happened to be attending a birth for a family from Huntsville, Alabama. When Brock told them about the cease-and-desist, they decided to help. “My husband and I really felt like the Lord called us to do it,” said a woman I’ll call Debbie, who asked to remain anonymous.
After months of searching, Debbie and her husband bought a three-bedroom house in southern Tennessee and enlisted friends and relatives to help convert it into a two bedroom, two bath.
They installed a capacious hot tub and an extra water heater. It is now one of about half a dozen birthing cottages scattered around the towns of St. Joseph, Elkton, Pulaski and Lawrenceburg. There is also a renowned midwifery center nearby in Summertown called The Farm, which has cottages that expecting families can rent. The Farm was originally founded as a commune in the 1970s by hippies who caravanned across the country from San Francisco in school buses. Many of the women in the caravan were pregnant and learned how to deliver each other’s babies, which inspired them to become midwives.

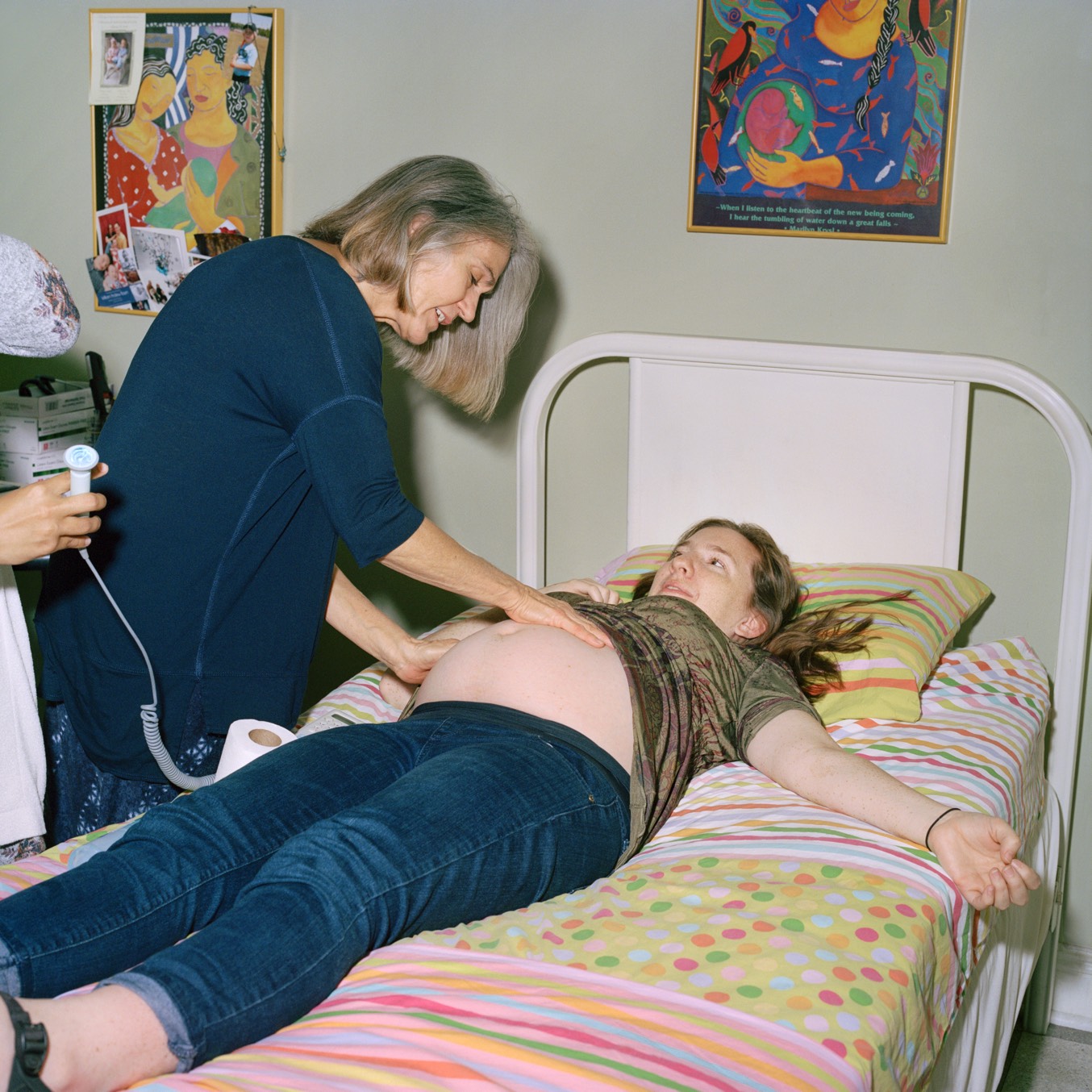


Alabama’s border birth community is a tightknit sisterhood. It includes engineers, meteorologists, nurses, real estate agents and stay-at-home moms of varying political persuasions. They drop terms like “proven pelvis” and “colostrum” into casual conversation and share information via word of mouth. The cottages don’t openly advertise their services, for fear of being identified as unlicensed birth centers.
In theory, any Airbnb or vacation property could be used as a birthing cottage, but there are benefits to using one within the network. The owners are supportive and flexible about booking. After a birth, Debbie and her family clean the house themselves. (“It’s hard to find someone and say, ‘There may be blood, you may need to wear gloves, and the tub needs to be disinfected,’” she explained.) The cottages, which cost anywhere from $250 to $1,500 a week, tend to be filled with the quaint, fusty furniture that inhabits secondary properties everywhere. One is affectionately known as the “barbershop house” because the owner also cuts hair in the garage. When Marie Douthit’s husband dropped off supplies there in preparation for his wife’s labor, he got a quick trim.
Douthit decided to jump the border after her first pregnancy resulted in a C-section that left her deeply distressed. A data-oriented engineer, she ran the numbers and concluded that a home birth with a midwife was less risky than another C-section in a hospital. She went into active labor for her second baby on January 18, 2017. On the way to the barbershop house, Douthit and her husband stopped to use the bathroom and get Douthit a Hardee’s milkshake. A convenience store clerk asked if she needed an ambulance, and Douthit, who was terrified of being taken to the hospital, rushed back to the car. When they reached the cottage, the midwives didn’t even have time to fill the tub all the way to the top before she felt the urge to push. Her baby was born an hour later.

Brianna Barker gave birth using the network around the same time. She’d had her first child at 20; the baby was preterm and breech. It was months after her C-section before she could even walk standing up straight; she still has recurring nightmares about being trapped in a dark hospital. She used birthing cottages for her third and fourth pregnancies. For one of them, her doula taught Barker and her husband how to do a car birth just in case the baby came during the two-and-a-half-hour drive.
One reason Barker opted to use a midwife was that many doctors and hospitals won’t allow women to give birth vaginally after a C-section, due to a widespread misconception that a vaginal birth after cesarean, or VBAC, is unsafe. In fact, VBACs are associated with fewer complications than elective repeat C-sections, according to the Mayo Clinic. The American College of Obstetricians and Gynecologists (ACOG) endorses their use for low-risk moms, although it doesn’t recommend VBACs outside a hospital environment and generally supports hospitals and accredited birth centers as a safer option than home birth.
There have been no large-scale randomized clinical trials of planned home birth that the ACOG considers adequate. Existing research suggests that in the U.S., they are associated with fewer interventions but also with higher rates of infant death. In countries like the Netherlands and Canada, however, where home birth is well established, it’s considered safe. A study that included researchers from the University of British Columbia; the Child and Family Research Institute in Vancouver; King’s College, London; and the University of Alberta, Edmonton compared planned home birth with planned hospital birth. The authors found that home birth was associated with “very low and comparable rates of perinatal death,” as well as fewer surgeries and complications for moms.
All 14 Alabama women I spoke to said their decision to jump the border was connected to their desire to avoid unnecessary medical procedures. Most of them described harrowing hospital experiences—being derided for writing a birth plan, feeling pressured into C-sections, epidurals or Pitocin, a synthetic hormone that induces contractions.
Alabama is one of nine states where more than 34 percent of deliveries are cesareans. The ideal, according to the World Health Organization, is 10 to 15 percent. While cesareans may be essential in complicated births, they can come with higher risks of (sometimes life-threatening) complications and infection. “You have to look at the outcomes from hospital births, and they are not that good,” said Dr. Jesanna Cooper, an obstetrician who works with nurse-midwives in her Birmingham practice. “If it’s risky to have a hospital birth, it’s pretty hard to say a home birth is too risky.”




The Pettys live a little way out of town, on a street with modest homes surrounded by large yards. When I spotted a massive camper parked in one, bearing a decal that said “The Baby Wagon,” I knew I’d found the right place.
Kate grew up in Alabama. She was a stubborn kid, never big on rule-following. She and Caleb met at a hole-in-the-wall pool hall in 2011. “I'm pretty good for a girl. I can kick a lot of people’s booties,” she told me proudly. She was initially wary when she learned Caleb was seven years younger, but they married in 2013, planning on a big family.
Kate started out as a “very mainstream mother,” she said, clipping coupons, using disposable diapers, buying processed food. Their first daughter, AdaRee, was born on March 1, 2014, at East Alabama Medical Center. Kate had an epidural but hated not being able to feel what was happening to her body. When she got pregnant less than a year later, she was determined to give birth without drugs or surgical interventions. After going into labor, she stayed at home for as long as she could, figuring she had a better chance of avoiding unwanted procedures that way. She arrived at the hospital 8 centimeters dilated—but then her labor stalled. A nurse insisted that she needed Pitocin. “I said no repeatedly,” Kate recalled. “I finally caved.”
After receiving Pitocin through an IV, Kate experienced swells of unrelenting pain. She felt like she was dying; the doctor gave her narcotic painkillers. The baby’s heart rate started to drop. The doctor used a vacuum to get the baby out fast and then put her on oxygen. Her name was Eliza, and Kate got to touch her face and her hand before they rolled her out of the room. Eliza died three hours later.
Kate’s instincts were screaming that Eliza’s death wasn’t supposed to happen. When she asked the doctor if her baby’s death was caused by the labor drugs, he dismissed that possibility, she said. (East Alabama Medical Center declined to comment.) The autopsy report attributed the death to respiratory failure and a possible infection, an explanation Kate felt was “ludicrous at best.” She sought opinions from three other obstetricians, none of whom blamed the Pitocin. According to Kate, an OB in Atlanta told her he thought that the heart strips in Kate’s medical records indicated a connection between the intensity of the Pitocin-induced contractions and the stress Eliza was under in the womb. “I can’t tell you how much of a weight he lifted off my shoulders,” Kate said. “It was the most spiritual moment of my life.” Soon after, Kate and Caleb started trying to have another baby.

Eliza’s death had made Kate question everything, from the food she ate to the products she bought. There was no way she was going back to the hospital. She considered traveling to Tennessee to The Farm or giving birth at a relative’s house in Chattanooga with a midwife, but the five-hour journey was too far. She couldn’t convince an out-of-state midwife to come to her home. As she hit her 20-week mark, she was becoming increasingly anxious.
Finally, a friend put her in touch with a Georgia-based midwife who was willing to assist Kate as long as the birth wasn’t in Alabama. Almost as a joke, Kate asked, “Look, what if I buy a camper?” To her surprise, the midwife said that as long as the camper was parked over the Georgia line, that was fine. So that’s what the Pettys did.
Kate believed that because Eliza’s birth had been so traumatic, God would take it easy on her the next time around. But every logistical detail presented a new obstacle. Finding an affordable RV, for instance. Kate was working as a part-time real estate agent and Caleb was running a granite shop, and they didn’t have great credit. They finally found a used camper for $17,000, which came with two used Jet Skis, and Kate’s mother co-signed the loan. Then, after they settled on 3 Creeks Campground, Kate discovered she couldn’t book a site in advance. So they drove the camper up a few days before Kate’s due date and paid for a week.
These hurdles prompted Kate to throw herself into a decades-long campaign to change Alabama’s law on midwives. A group of activists led by the Alabama Birth Coalition spent so much time at the statehouse that they knew the best bathrooms for impromptu meetings and breastfeeding (the seventh floor). Brianna Barker took her infant along when she lobbied state lawmakers. Kate showed up into her ninth month of pregnancy and went back after Jett’s birth.
On May 19, 2017, the Alabama Legislature passed a bill allowing certified professional midwives to practice. But because of heavy opposition from the medical establishment, the bill came with numerous exclusions. When the law goes into effect—which is expected to happen before the end of 2018—midwives will not be able to attend mothers who have had C-sections or who are giving birth to twins or breech babies. Given the state’s high C-section rates, this rules out at least 35 percent of Alabama moms. “It was a gut punch,” Barker said.

Because of the law’s many exceptions, the border birth ecosystem will remain in place. And for the foreseeable future, midwife care is likely to be a viable option mostly for white women of some means. Melodi Stone, a black doula and reproductive justice advocate in Birmingham, said that because black women’s pregnancies are more likely to be high-risk (they have greater incidence of obesity, high blood pressure and other factors), they may not qualify to give birth at home with midwives. Even if they are eligible, the cost is expected to remain a deterrent for many. There are no plans for midwifery to be subsidized by Medicaid, which, as of 2016, covered 58 percent of births in Alabama. Health insurance providers also rarely cover midwifery care, which costs at least $3,000 (not counting the added expenses of jumping the border).
This is unfortunate because black mothers could especially benefit from a dedicated advocate during the birth process. Nationally, black women are more than twice as likely to die from pregnancy-related causes as white women. In Alabama, they are five times as likely. In 2016, the infant mortality rate for black infants in the state was more than double that of white infants. But after four decades without legal midwifery in Alabama, many black women aren’t even aware it’s an option. “This was knowledge supposed to be passed down, but there’s a lot of misinformation out there, and information that we don’t have has been stolen from us,” said Kendra Burrell, a doula in Alabama. “I thought midwifery was literally a white woman thing.”
Kate hopes to eventually train as a midwife. In recent months, she has been acting as a doula for Erin Inman, a young mother she met on Facebook who lives in nearby Phenix City. Inman is due to give birth to her second baby in February. Like so many other border moms, she had a C-section for her first pregnancy that she still struggles with. Kate offered the use of her camper, but Inman wanted somewhere that could more easily accommodate a birthing tub. So Kate is researching hotel rooms in LaGrange, Georgia, an hour away from Inman’s home—not an easy task, because hotel websites often don’t include photos of bathrooms and it’s hard to tell the size of the room or the thickness of the walls.
Kate and Inman plan to drive to LaGrange and request room tours when Inman approaches 36 weeks. They won’t book a room until she goes into labor, though, because Inman doesn’t want to pay for more nights than she has to. She’s a little nervous that someone in a neighboring room might hear odd noises and call the police. But that still worries her less than going to a hospital.
As for Kate, she and Caleb can’t wait to have another baby. She may even use the camper again, which has come to represent something sacred for the Pettys: a refuge and a source of healing. Jett has a forest green “Born in a Camper” cloth diaper and his first birthday party had a “Happy Camper” theme. Kate’s parents and brother bought RVs of their own (her sister already owned one) and the whole family takes them on trips. “People look at me like I’m crazy when I say I chose home birth as the safer option,” Kate said. “If I had that with AdaRee and Eliza, my family would be whole. There’s no doubt in my mind. If I had stayed home that day or had a midwife, Eliza would be here with us right now.”